
Various factors influence the cost of therapy for obstructive sleep apnea, including the treatment option prescribed and the patient’s insurance provider. The cost of diagnostics varies as it depends on whether you want to take a sleep study at home or at a sleep center, and the treatment for sleep apnea will vary depend on how severe the sleep disorder is.
In Fairview, TX, Dr. Tina Feng and her team can work with your insurance provider to help optimize your coverage as well as arrange financing to cover any leftover out-of-pocket costs. People who suffer from obstructive sleep apnea have a higher risk of developing high blood pressure, heart disease, and other significant health conditions; thus, it is well worth getting treatment right away.
An overnight sleep study, also known as a polysomnogram (PSG), is a common diagnostic tool used to identify the cause of breathing problems while sleeping. The polysomnogram is a sleep test that records, monitors, and analyzes brain waves, heart rate, breathing patterns, and muscle movements. It helps the sleep physician determine if you have sleep apnea and how severe it is.
The approximate cost of this exam depends on the location where the patient takes the exam and whether your medical insurance covers the test. To treat OSA, you must undergo an overnight polysomnogram exam and have a sleep doctor review the report before any sleep apnea treatment can begin. The cost of a sleep study varies by insurance coverage and type of study. A professional sleep study at a medical facility costs approximately $0-$2500, but is generally covered by insurance. If you take a home sleep study, the cost is between fully covered to around $250. If you don’t have insurance and plan to take the sleep study at a medical facility, the cost will vary between $2,000 and $3,000.
To ensure that your insurance company covers the cost of your dental sleep apnea device, you need to have a sleep study or sleep specialist diagnose the condition. In most cases, dental insurance does not cover a dental appliance or a CPAP; however, your medical health insurance company may cover the cost because it’s designed to help with a medical issue, not a dental one. While everyone’s specific plan is different, oral devices are typically covered by health insurance plans.
It is recommended to contact your insurance provider to know your benefits to understand what is and what isn’t covered in your policy. If you need third-party financing, we’re partnered with CareCredit and LendingPoint to help you budget for any out-of-pocket expenses. We can also help you navigate the requirements of your insurance plan.
When it comes to treating mild sleep apnea or severe sleep apnea, there are a few distinct options to treating sleep apnea, each with its own set of costs. The cost for sleep apnea treatment varies as it depends on your insurance coverage or whether you are paying out of pocket with no insurance.
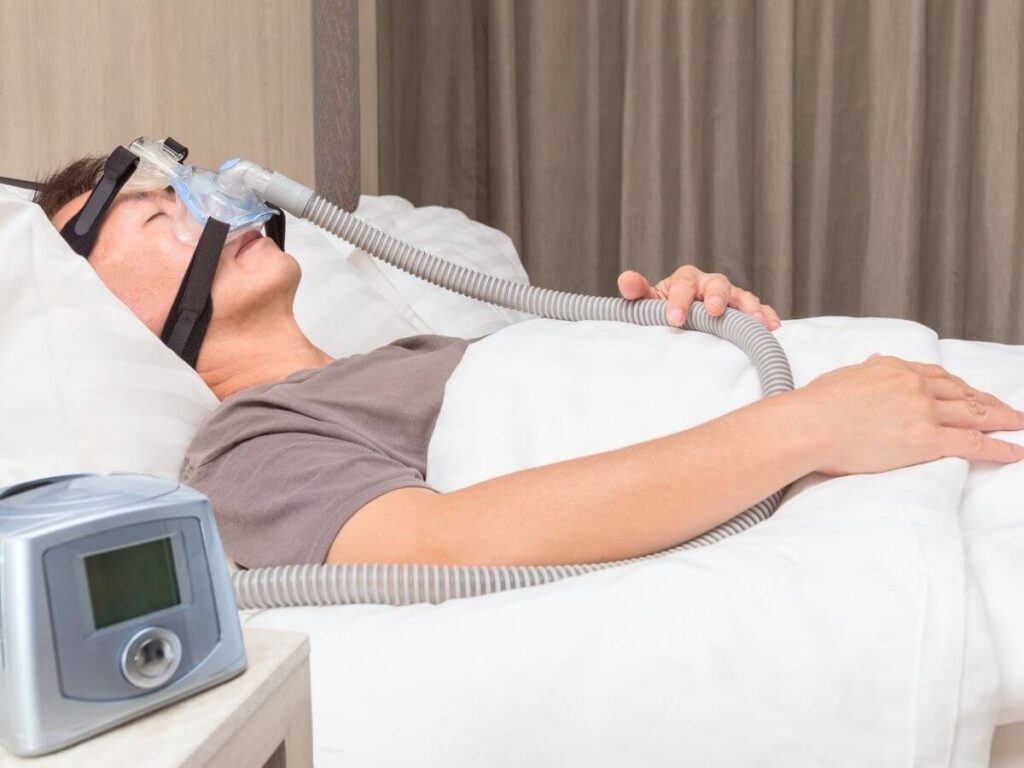
The use of continuous positive airway pressure (CPAP) devices are among the most frequent treatments for patients with severe sleep apnea. Many doctors feel that the CPAP treatment is critical therapy for their obstructive sleep apnea patients. It comprises a mask that produces a constant stream of air while sleeping to maintain airways openings throughout the night.
The average cost for a CPAP device can start as low as $500 to upwards of $2,000 or more depending on the device and its features. When using a CPAP device, it requires accessories that needs to be replaced or maintained to prevent bacterial growth and to ensure that your machine is working correctly. Some health insurance companies will cover the cost of these devices if they are medically essential, but not replacement costs.
The device improves breathing and may increase the overall health of the patient. However, CPAP therapy has several drawbacks. Some patients find it uncomfortable to wear a mask, are noisy, feel embarrassed wearing a mask, and have difficulty tolerating forced air. In addition, every night the patient must be wired to the device, making some feel restricted.
If you’re experiencing these issues with your machine and do not have severe sleep apnea, you may benefit from switching to the more modern alternative known as the oral appliance system (OAS). Patients using OAS generally have moderate obstructive sleep apnea, and the device works like a mouth guard worn at night. The device is comfortable, less intrusive than CPAP machines, and even easier to use.
To decrease or tighten extra tissue, your doctor may use laser therapy. The procedure is non-invasive and is generally done over multiple sessions. The cost may vary depending on the severity of the case but generally ranges from $2,500 – $4,000. The benefit of using laser therapy for sleep apnea is that you do not need to sleep with a CPAP mask or an oral dental appliance.
An oral appliance, also known as a dental appliance, sleep apnea dental device, or oral device, is a non-invasive cost-effective way to treat mild to moderate sleep apnea disorder. Oral devices for sleep apnea therapy (if CPAP is not tolerated or does not work) are often used as an alternative treatment to CPAP or sleep apnea surgery. When using a sleep apnea dental appliance, it is a removable dental device that keeps your upper airway open and helps you breathe more easily when you sleep.
The average sleep apnea oral appliance cost depends on the particular type of dental appliance mouthpiece and on each patient’s individual needs. The cost is generally between $2,000-$3,000 and is usual for treatment to cover the actual mouthpiece itself and the dental visit, adjustments, follow-up visits, and any modifications to the dental device required. Health insurance and Medicare generally cover oral appliances for sleep apnea since they are essential for better health.
Patients who experience severe obstructive sleep apnea with high or severe breathing obstruction levels are generally not candidates for oral appliances. However, sleep physicians may also discuss alternative forms of treatment, such as Continuous Positive Airway Pressure (CPAP), for these patients if their OSA is resistant to the usual efficacious treatment.

There are numerous advantages for patients who use a sleep apnea dental appliance. Among these advantages are the following:
Yes, you can skip using a CPAP machine and start oral appliance therapy as a treatment option to help control moderate sleep apnea. Using the dental appliance can prevent snoring and allow the airway to remain open even while you’re sleeping.
Sleep apnea is a serious condition that doesn’t go away on its own, which means you’re not getting a good night’s rest and enough oxygen. If left untreated, it can lead to daytime fatigue, teeth grinding and other serious health problems such as heart trouble, diabetes, stroke, or high blood pressure.
In general, over-the-counter oral devices should not be used for obstructive sleep apnea treatment. In certain situations, OTC oral devices might force the jaw in a worse position for the airway. Without the proper treatment and supervision from a doctor, there are no benefits to these devices that outweigh the risks associated with using them.
Treatment for sleep apnea will vary from person to person as it will depend on how severe their sleep apnea is. The most common sleep apnea oral devices are:
At Sloan Creek Dental, we believe you deserve a good night’s sleep. If you are interested in learning more about the cost of treating sleep apnea treatment, how you can get a dental appliance for sleep apnea, or how we go about treating sleep apnea, contact our office online or call us at 972-468-1440, or leave us a message.
Our dental office is located in Fairview, Texas, and our sleep apnea patients visit us from across the surrounding areas, including Allen, Plano, McKinney, and Lucas.
We firmly believe that the internet should be available and accessible to anyone, and are committed to providing a website that is accessible to the widest possible audience, regardless of circumstance and ability.
To fulfill this, we aim to adhere as strictly as possible to the World Wide Web Consortium’s (W3C) Web Content Accessibility Guidelines 2.1 (WCAG 2.1) at the AA level. These guidelines explain how to make web content accessible to people with a wide array of disabilities. Complying with those guidelines helps us ensure that the website is accessible to all people: blind people, people with motor impairments, visual impairment, cognitive disabilities, and more.
This website utilizes various technologies that are meant to make it as accessible as possible at all times. We utilize an accessibility interface that allows persons with specific disabilities to adjust the website’s UI (user interface) and design it to their personal needs.
Additionally, the website utilizes an AI-based application that runs in the background and optimizes its accessibility level constantly. This application remediates the website’s HTML, adapts Its functionality and behavior for screen-readers used by the blind users, and for keyboard functions used by individuals with motor impairments.
If you’ve found a malfunction or have ideas for improvement, we’ll be happy to hear from you. You can reach out to the website’s operators by using the following email
Our website implements the ARIA attributes (Accessible Rich Internet Applications) technique, alongside various different behavioral changes, to ensure blind users visiting with screen-readers are able to read, comprehend, and enjoy the website’s functions. As soon as a user with a screen-reader enters your site, they immediately receive a prompt to enter the Screen-Reader Profile so they can browse and operate your site effectively. Here’s how our website covers some of the most important screen-reader requirements, alongside console screenshots of code examples:
Screen-reader optimization: we run a background process that learns the website’s components from top to bottom, to ensure ongoing compliance even when updating the website. In this process, we provide screen-readers with meaningful data using the ARIA set of attributes. For example, we provide accurate form labels; descriptions for actionable icons (social media icons, search icons, cart icons, etc.); validation guidance for form inputs; element roles such as buttons, menus, modal dialogues (popups), and others. Additionally, the background process scans all of the website’s images and provides an accurate and meaningful image-object-recognition-based description as an ALT (alternate text) tag for images that are not described. It will also extract texts that are embedded within the image, using an OCR (optical character recognition) technology. To turn on screen-reader adjustments at any time, users need only to press the Alt+1 keyboard combination. Screen-reader users also get automatic announcements to turn the Screen-reader mode on as soon as they enter the website.
These adjustments are compatible with all popular screen readers, including JAWS and NVDA.
Keyboard navigation optimization: The background process also adjusts the website’s HTML, and adds various behaviors using JavaScript code to make the website operable by the keyboard. This includes the ability to navigate the website using the Tab and Shift+Tab keys, operate dropdowns with the arrow keys, close them with Esc, trigger buttons and links using the Enter key, navigate between radio and checkbox elements using the arrow keys, and fill them in with the Spacebar or Enter key.Additionally, keyboard users will find quick-navigation and content-skip menus, available at any time by clicking Alt+1, or as the first elements of the site while navigating with the keyboard. The background process also handles triggered popups by moving the keyboard focus towards them as soon as they appear, and not allow the focus drift outside of it.
Users can also use shortcuts such as “M” (menus), “H” (headings), “F” (forms), “B” (buttons), and “G” (graphics) to jump to specific elements.
We aim to support the widest array of browsers and assistive technologies as possible, so our users can choose the best fitting tools for them, with as few limitations as possible. Therefore, we have worked very hard to be able to support all major systems that comprise over 95% of the user market share including Google Chrome, Mozilla Firefox, Apple Safari, Opera and Microsoft Edge, JAWS and NVDA (screen readers), both for Windows and for MAC users.
Despite our very best efforts to allow anybody to adjust the website to their needs, there may still be pages or sections that are not fully accessible, are in the process of becoming accessible, or are lacking an adequate technological solution to make them accessible. Still, we are continually improving our accessibility, adding, updating and improving its options and features, and developing and adopting new technologies. All this is meant to reach the optimal level of accessibility, following technological advancements. For any assistance, please reach out to